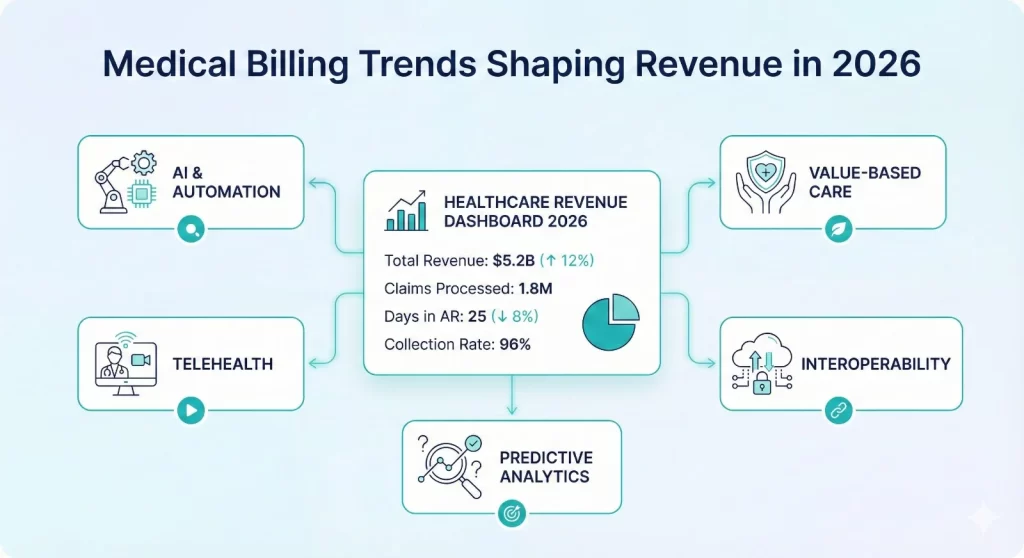
The management of healthcare revenue is undergoing significant shifts. From artificial intelligence that streamlines claims processing to the introduction of new rules for billing telehealth, medical billing trends in 2026 are fundamentally altering the way providers make money and optimize cash flow. These changes are a strategic redesign of the entire revenue cycle. For medical office administrators and billing professionals, knowing these changes is crucial to ensuring the financial stability of the business while providing quality medical care.
Artificial intelligence has evolved from being an experimental technology to a vital infrastructure for medical billing procedures. AI-powered systems can now examine hundreds of claims within just a few minutes and identify coding errors, insufficient documentation, and potential denials before submission. Machine learning algorithms analyze patterns of denials from specific payers in the past, enabling billing teams to anticipate issues that have previously caused rejections.
Natural language processing scans medical documentation and recommends accurate CPT and ICD codes, which dramatically reduce human error. One healthcare facility has reported a 68% decrease in workflow costs and a 72% increase in response times following the introduction of automated robotic processes. These systems can handle repetitive tasks, such as verifying eligibility and posting payments, allowing professionals to concentrate on cases that require judgment and expertise.
AI-driven predictive analytics can now accurately predict claims that are most likely to be subject to risk of denial, enabling preemptive corrections. Certain advanced platforms have increased the first-pass acceptance rate of claims to 95%, thereby directly enhancing the flow of cash and reducing the administrative burden of appeals, as well as the need for resubmissions.
The shift from fee-for-service to value-based healthcare is one of the biggest medical billing trends reshaping revenue cycle management. Medicare, Medicaid, and commercial payers are increasingly offering value-based agreements that prioritize the quality of care over volume. This change will require billing departments to monitor a complete variety of indicators.
Instead of charging for specific procedures, doctors are now reporting on quality metrics such as hospital readmission rates, chronic disease management outcomes, and patient satisfaction scores. Bundled payments replace the itemized costs for care events, which require sophisticated tracking systems that link the clinical outcomes to the financial performance.
Healthcare providers must be able to document and prove significant improvements in healthcare for patients to be eligible for incentive programs or to avoid penalties. The billing process has become more complex, requiring the integration of medical documentation, quality reporting, and the financial system.
The automation of processes by robotics has revolutionized the time-consuming aspects of medical billing. RPA robots now manage patient registration, insurance verification, claim submission, payment posting, and denial management without human intervention. What was once a process that required hours of manual entry now takes place in just a few minutes, with higher precision.
Healthcare facilities that utilize RPA have reported significant efficiency gains. One health system has eliminated $13 billion in manual claims status checks within a single year. The technology excels at rules-based tasks that follow regular patterns. When combined with AI, RPA systems can handle more complex decisions and also learn from data patterns to improve their performance over time.
Telehealth billing has evolved from pandemic-related emergency measures into permanent revenue cycle elements. The Centers for Medicare & Medicaid Services confirmed that Place of Service code 10 remains active for telehealth services at home until 2026. Telehealth services that are audio-only have been permanently extended to the behavioral and mental health sector, even when audio-video capabilities are not available.
Providers must learn about new coding requirements. Telehealth claims require the precise use of modifiers, including modifier 95 for synchronous video visits and modifier 93 for audio-only visits, as well as the accurate location of Service codes. The requirements for documentation have been progressively stricter, with payers demanding proof that audio-video services were provided, but not being able to bill only audio services.
Remote patient monitoring represents a growing reimbursement opportunity. CPT codes 99453, 99454, 99457, and 99458 permit companies to charge for the setup of devices, monthly data transmission, and interactive care management. A proper billing process requires, at a minimum, 16 days of data collection per month and complete documentation of medical necessity. For practices with 100 RPM patients, accurate billing could result in approximately $ 110,000 in annual reimbursement.
Predictive analytics tools analyze historical billing data to identify patterns that lead to claim denials, enabling organizations to resolve issues before claims are submitted. These systems flag claims with high risk due to specific CPT codes that certain payers frequently reject, highlight gaps in documentation that consistently cause rejections, and also identify timing or authorization issues that impact the approval rate.
Data analytics has also transformed auditing processes. The Centers for Medicare & Medicaid Services utilizes sophisticated algorithms to identify coding irregularities and incorrect billing patterns. Healthcare providers who use similar analysis internally can identify revenue leakage and compliance risks before external auditors do. This proactive approach helps protect companies from financial penalties while maximizing legal revenue collection.
Prior authorization has historically been one of the most difficult bottlenecks in healthcare delivery. Approximately 70 percent of previous authorization processes rely on manual labor, but the advent of automation is rapidly transforming the landscape.
AI-powered prior authorization systems extract the necessary clinical information from electronic medical records, automatically review the payer requirements, and then submit authorization requests through the proper channels. The systems can automate up to 82 percent of workflows for prior authorization, as well as manage 1.3 million regulations across more than 300 health insurance plans.
When payers request additional information, AI agents analyze patient data and generate precise, evidence-based responses with minimal human intervention. This reduces the time from authorization request to delivery of care from days to just a few hours, thereby directly improving patient outcomes and decreasing administrative burden.
As patient responsibility has become the third largest payer category in healthcare, providers need to provide clear cost transparency and flexible payment options. Research shows that 46% of patients decide to stop treatment after receiving estimates of high costs, and 60% consider switching providers following unexpected charges or inaccurate estimates.
Advanced cost estimator tools for patients offer accurate out-of-pocket estimates before the services are performed. These systems review the previous payment history for facility and physician fees, as well as the individual’s benefit information, to create personalized estimates. Transparency upfront increases patient trust, improves upfront collections, and reduces billing disputes.
Healthcare facilities are creating patient portals that provide secure access to bill information, itemized bills, and flexible payment options. Automated appointment reminders may include cost estimates and facilitate the collection of initial payment before service delivery. Financial engagement that is proactive shifts the conversation from post-service collection concerns towards pre-service preparation.
Interoperability in healthcare, particularly through Fast Healthcare Interoperability Resources, is transforming the way billing systems communicate. FHIR utilizes modern web standards, including JSON, RESTful APIs, and XML, to facilitate efficient information exchange between electronic health records, billing platforms, and payer systems.
The Centers for Medicare & Medicaid Services and the Office of the National Coordinator have approved FHIR R4 as the standard for exchanging healthcare data. This enables real-time eligibility verification, immediate claim status updates, and automated remittance processing. If billing information flows smoothly across different platforms, claims can be processed more efficiently and with fewer errors, thereby reducing administrative costs and shortening reimbursement times.
Many healthcare companies are outsourcing their medical billing services to companies that offer high-end technology, certified coders, and expertise in meeting a variety of payer demands. Outsourcing can reduce operational costs by 30-40% and increase the rate of collection to around 95%..
Outsourced billing providers offer flexibility that in-house departments often struggle to maintain. As practices expand their locations or specialties, or increase the number of patients they see, outsourcing firms can adjust their resources without having to recruit, hire and train new staff.
The best outsourcing partners provide transparency by regularly reporting key metrics, including the collection ratio, first-pass payment rates, and denial percentages. The most effective outsourcing relationships are collaborations between billing specialists and clinical teams, ensuring accurate coding and maximizing reimbursement.
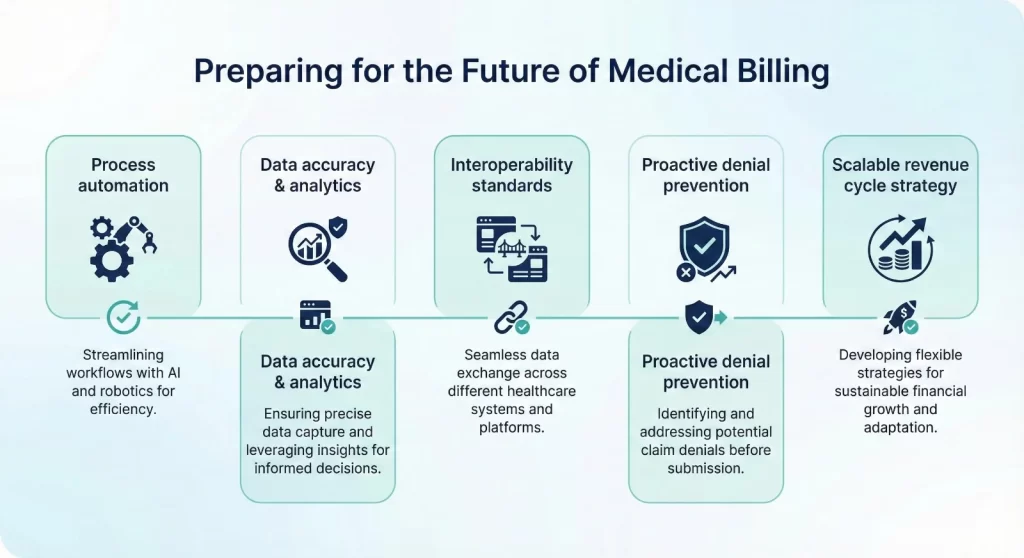
Healthcare organizations that will be financially successful over the next 2026 years will take on the current medical billing trends strategically rather than reacting. To succeed, they must invest in the latest technology platforms, provide extensive staff training, and dedicate themselves to continually improving processes.
Begin by evaluating the current denial rates and identifying the most frequent reasons for rejections. Implement AI-powered claim scrubbing to remove procedures with high denial rates. Establish clear telehealth billing guidelines to ensure proper use of modifiers and documentation. Utilize predictive analytics tools to identify revenue leakage before it impacts cash flow.
Revenue integrity should be a strategic goal that connects clinical documentation, coding accuracy, and billing compliance into a unified system. Regular internal audits help identify systematic problems before they lead to the enforcement of external laws or the loss of revenue.
The landscape of medical billing is expected to continue evolving in response to technological advancements, regulatory changes, and shifting payment models. Companies that are well-informed, agile, flexible and proactive will be in a position to achieve long-term financial growth while providing outstanding patient care.