
For many Kaiser Permanente plans that cover doula services, payment is tied to using a Kaiser‑contracted doula listed in the Kaiser doula directory. If the doula is not contracted (or the member’s plan requires contracted providers), the service may be considered non‑covered meaning the claim can deny and the doula will not be paid. To avoid preventable denials, doulas should confirm plan rules, complete Kaiser’s provider enrollment/contracting requirements, and submit claims with the required identifiers and documentation.
Kaiser Permanente’s doula benefit has expanded, but coverage rules are strict: many plans require members to use doulas who are contracted with Kaiser and listed in Kaiser’s doula directory. When a service is “not covered,” claims are commonly denied creating delays, rework, and missed revenue for doulas and billing teams.
Key takeaway: if you’re serving Kaiser members, make contracting and eligibility verification part of your standard intake before you provide services.
In insurance billing, coverage drives payment. If a plan covers doula services only when they are delivered by a contracted provider, a non‑contracted doula claim is likely to deny as non‑covered. Even when a plan has out‑of‑network pathways, documentation and payer rules can still create payment risk.
Scenario | What happens | Payment risk |
Member’s plan requires Kaiser‑contracted doulas | Non‑contracted services treated as non‑covered | High (denial/non‑payment) |
Doula is contracted but claim is missing required identifiers | Claim rejected or pended for info | Medium (delay) |
Doula is contracted + clean claim submitted | Normal adjudication + faster payment | Low |

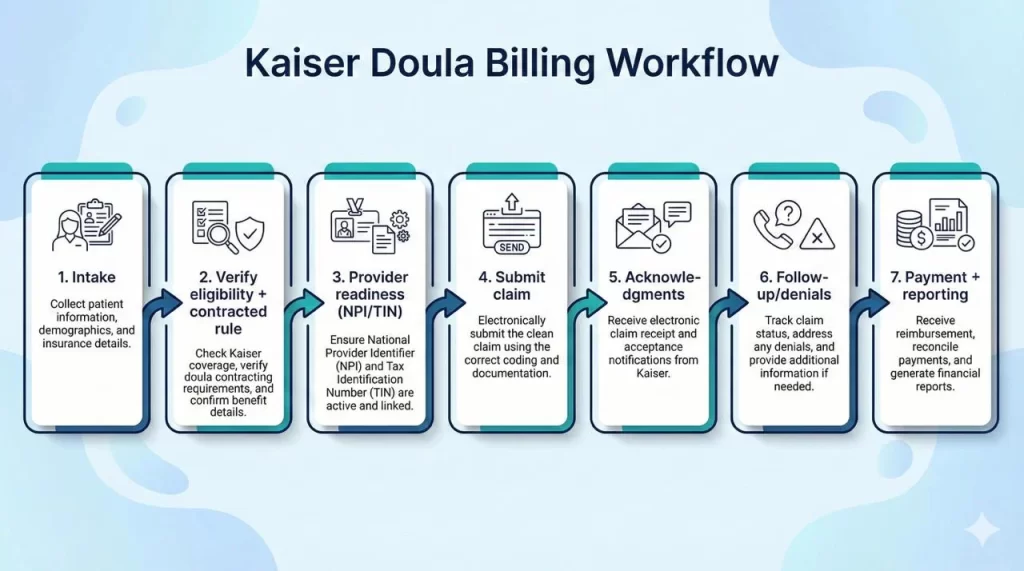
“Contracted” and “enrolled” are often used interchangeably, but in billing they can mean different steps. For Kaiser doula billing, think of it as: (1) eligibility/coverage rules, (2) provider contracting (if required), and (3) provider enrollment details needed on claims.
Most payment problems are preventable when the front‑end steps are consistent. Here are common drivers and the fix.
Issue | Why it happens | Prevention step |
Non‑covered/non‑contracted provider | Plan requires contracted doula for coverage | Verify plan coverage rules at intake + confirm directory/contract status |
Missing/incorrect identifiers | NPI/TIN or billing fields incomplete | Pre‑submission checklist + standardized claim templates |
Claim format errors | Incorrect CMS‑1500 fields or coding/units | QA review before submission + batch validation |
Late filing | No follow‑up cadence; rejections not cleaned quickly | A/R worklists + rejection cleanup within 24–72 hours |
Documentation mismatch | Visit type billed not supported by note | Use a documentation checklist by visit type |

Keep documentation simple, consistent, and aligned to what is billed. A lightweight checklist prevents downstream denials.
Metric | Why it matters | Goal |
First‑pass acceptance rate | Measures claim cleanliness | Increase over time |
Rejection rate + top errors | Shows data/format issues | Drive toward near‑zero |
Denials by category | Reveals preventable revenue leaks | Reduce non‑covered/contracting and missing‑info denials |
A/R aging buckets | Shows cash flow health | Keep older aging under control |
Turnaround time to payment | Measures collection speed | Shorten with consistent follow‑up |
Need help getting your Kaiser doula billing workflow set up (or fixing denials that are already aging)? Contact Claim N Billing to review your contracting readiness, claim templates, and follow‑up process so you can reduce denials and get paid faster.