A busy medical office requires juggling the needs of patients, coordinating staff, and managing the endless paperwork necessary to keep things running smoothly. If you’ve ever sat in front of a pile of rejected claims or wondered why reimbursements are taking so long, insurance credentialing is likely at the base of the problem. This process validates your provider’s qualifications, allowing them to be paid by insurers promptly. If you don’t have this, even the finest care won’t result in regular revenue. Let’s pretend we’re talking over a quick coffee break. As a manager, you’ll need practical guidance, not just words.
Consider the possibility of a new doctor joining your team. They have the expertise, but until large payers credential them, they’re out of network. Patients have to pay more out of pocket, or, even more importantly, they seek care elsewhere. Insurance credentialing bridges this gap by verifying qualifications, education, and history through organizations such as CAQH, as well as CMS. It’s not a choice, but it is the first step in joining networks like Medicare or Humana, where the majority of your billing is processed.
What Exactly Is Insurance Credentialing?
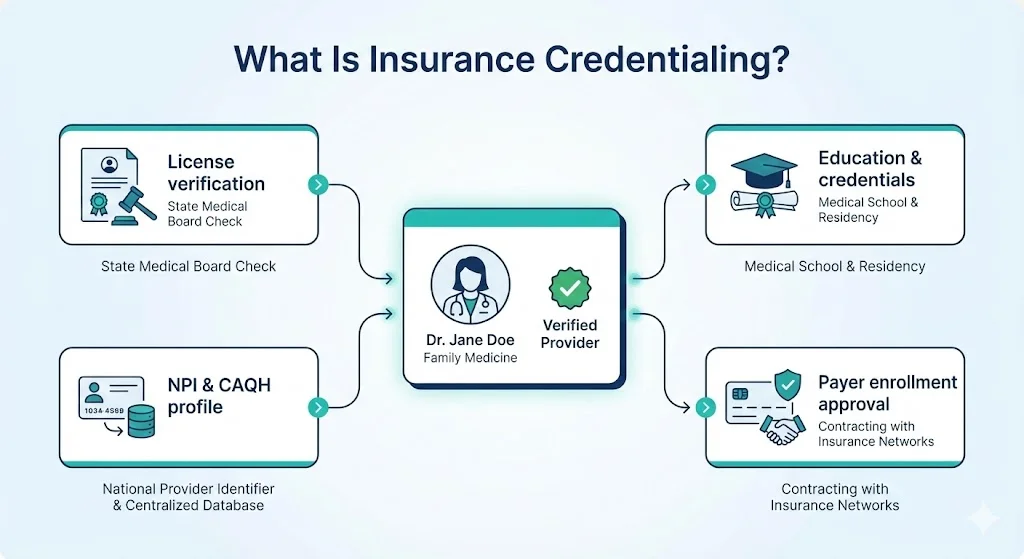 At its core, insurance credentialing is a process by which payers verify that providers meet specific standards before approving reimbursement. It’s a thorough check of credentials degrees, board certifications, malpractice history, and more – to protect patients and maintain quality. For instance, an office of a family physician in Texas may need to verify the physician’s NPI (National Provider Identifier) and submit the information via CAQH. This central database allows the sharing of information with multiple insurance companies.
Credentialing is directly linked to compliance with federal regulations issued by the Centre’s for Medicare & Medicaid Services (CMS). If you fail to follow the rules, you may be subject to fines or audits. If you do it right and your Practice will gain access to larger patient pools, which boosts both your image and bottom line. Imagine receiving a badge that reads, “We’re vetted and ready to serve.”
Providers, such as physicians, nurse practitioners, and therapists, are all subject to this. For group practices, it extends to the entire facility, ensuring that everyone is aligned with the payer’s contract. The U.S. healthcare system, where private insurers are the dominant force alongside government programs, being accredited allows you to be open to a variety of reimbursements.
At its core, insurance credentialing is a process by which payers verify that providers meet specific standards before approving reimbursement. It’s a thorough check of credentials degrees, board certifications, malpractice history, and more – to protect patients and maintain quality. For instance, an office of a family physician in Texas may need to verify the physician’s NPI (National Provider Identifier) and submit the information via CAQH. This central database allows the sharing of information with multiple insurance companies.
Credentialing is directly linked to compliance with federal regulations issued by the Centre’s for Medicare & Medicaid Services (CMS). If you fail to follow the rules, you may be subject to fines or audits. If you do it right and your Practice will gain access to larger patient pools, which boosts both your image and bottom line. Imagine receiving a badge that reads, “We’re vetted and ready to serve.”
Providers, such as physicians, nurse practitioners, and therapists, are all subject to this. For group practices, it extends to the entire facility, ensuring that everyone is aligned with the payer’s contract. The U.S. healthcare system, where private insurers are the dominant force alongside government programs, being accredited allows you to be open to a variety of reimbursements.
The Importance of Insurance Credentialing in Medical Billing
Do you really need to bother about all this? The answer is simple: it directly affects the cash flow. Providers with a valid credential can charge in-network rates, which are more stable and less expensive than out-of-network rates. If they don’t have it, claims are rejected, resulting in revenue losses that could reach 20-30% in certain practices. This is real money. Think delay in payment for routine procedures or visits.
Beyond finances, credentialing helps build trust. Patients prefer providers in-network to reduce costs, and thus having a credential increases your reach. It also ensures compliance, which reduces the risk of legal liability from organizations such as the Joint Commission. In a post-pandemic era where telehealth has experienced significant growth, the need for credentialing ensures that remote providers comply with state-specific guidelines and ensures the safety of your operations.
Find a small pediatric clinic. Through credentialing with Medicaid, they can access government-funded health care for families with low incomes, as well as ensuring stability in income while helping the community. It’s not just about billing; it’s about delivering quality healthcare without financial burdens. Additionally, with increasing scrutiny of fraud, possessing the proper credentials can help protect your practice from potential penalties.  At its core, insurance credentialing is a process by which payers verify that providers meet specific standards before approving reimbursement. It’s a thorough check of credentials degrees, board certifications, malpractice history, and more – to protect patients and maintain quality. For instance, an office of a family physician in Texas may need to verify the physician’s NPI (National Provider Identifier) and submit the information via CAQH. This central database allows the sharing of information with multiple insurance companies.
Credentialing is directly linked to compliance with federal regulations issued by the Centre’s for Medicare & Medicaid Services (CMS). If you fail to follow the rules, you may be subject to fines or audits. If you do it right and your Practice will gain access to larger patient pools, which boosts both your image and bottom line. Imagine receiving a badge that reads, “We’re vetted and ready to serve.”
Providers, such as physicians, nurse practitioners, and therapists, are all subject to this. For group practices, it extends to the entire facility, ensuring that everyone is aligned with the payer’s contract. The U.S. healthcare system, where private insurers are the dominant force alongside government programs, being accredited allows you to be open to a variety of reimbursements.
At its core, insurance credentialing is a process by which payers verify that providers meet specific standards before approving reimbursement. It’s a thorough check of credentials degrees, board certifications, malpractice history, and more – to protect patients and maintain quality. For instance, an office of a family physician in Texas may need to verify the physician’s NPI (National Provider Identifier) and submit the information via CAQH. This central database allows the sharing of information with multiple insurance companies.
Credentialing is directly linked to compliance with federal regulations issued by the Centre’s for Medicare & Medicaid Services (CMS). If you fail to follow the rules, you may be subject to fines or audits. If you do it right and your Practice will gain access to larger patient pools, which boosts both your image and bottom line. Imagine receiving a badge that reads, “We’re vetted and ready to serve.”
Providers, such as physicians, nurse practitioners, and therapists, are all subject to this. For group practices, it extends to the entire facility, ensuring that everyone is aligned with the payer’s contract. The U.S. healthcare system, where private insurers are the dominant force alongside government programs, being accredited allows you to be open to a variety of reimbursements.
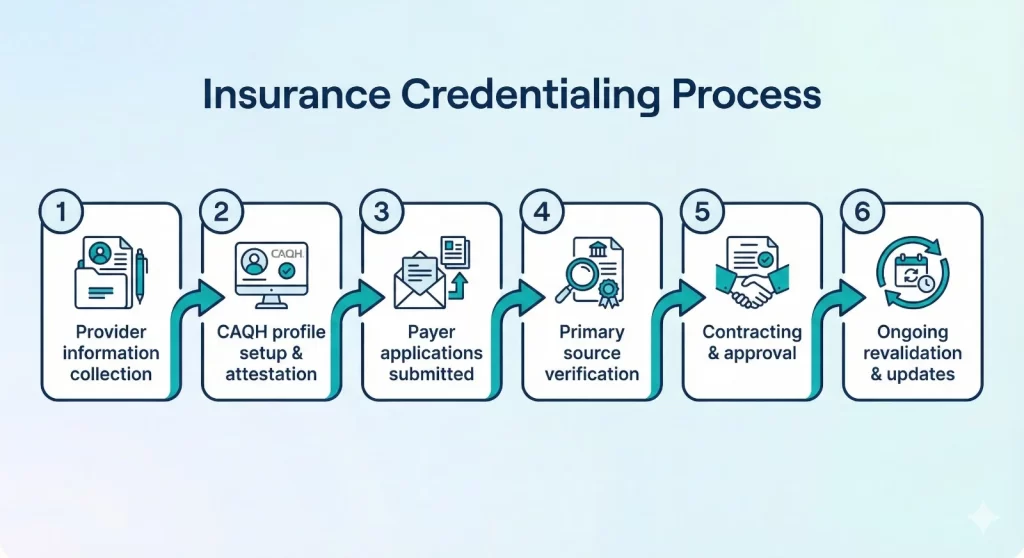 It can be overwhelming to begin, but breaking it down into small steps makes it easier. Begin by gathering the necessary documents, including diplomas and licenses, DEA registration, and proof of malpractice insurance. The accuracy of this information is crucial. Any error can delay everything.
Then, sign up for CAQH ProView, the preferred platform for the majority of payors. Upload your data once, and then allow insurers to access it. This reduces redundancy and saves hours. Apply this to specific payors. For Medicare, you can use PECOS (Provider Enrollment, Chain, Ownership, and Supply) to complete forms for private plans, such as Aetna.
Primary source verification is the next step, in which the payers verify the originals from boards or schools. It can take between 30 and 180 days, so be prepared for new employees. Once you’ve been approved, sign the contracts that outline the terms and rates. Please keep it in force for a period of 2 to 3 years. And update any changes to shifts in address quickly.
Imagine you are on the way to a specialist. Begin early, keep track of deadlines using a spreadsheet and then follow up every week. Tools such as CAQH simplify this process; however, perseverance will pay off.
It can be overwhelming to begin, but breaking it down into small steps makes it easier. Begin by gathering the necessary documents, including diplomas and licenses, DEA registration, and proof of malpractice insurance. The accuracy of this information is crucial. Any error can delay everything.
Then, sign up for CAQH ProView, the preferred platform for the majority of payors. Upload your data once, and then allow insurers to access it. This reduces redundancy and saves hours. Apply this to specific payors. For Medicare, you can use PECOS (Provider Enrollment, Chain, Ownership, and Supply) to complete forms for private plans, such as Aetna.
Primary source verification is the next step, in which the payers verify the originals from boards or schools. It can take between 30 and 180 days, so be prepared for new employees. Once you’ve been approved, sign the contracts that outline the terms and rates. Please keep it in force for a period of 2 to 3 years. And update any changes to shifts in address quickly.
Imagine you are on the way to a specialist. Begin early, keep track of deadlines using a spreadsheet and then follow up every week. Tools such as CAQH simplify this process; however, perseverance will pay off.