Provider Credentialing Services
What Are Provider Credentialing Services?
Provider credentialing services help healthcare providers and small clinics complete the paperwork and verification steps needed to join insurance networks. A complete credentialing program typically includes CAQH profile setup and maintenance, payer enrollment applications, follow-up to approval, effective date tracking, and ongoing re-credentialing so your network participation stays active.

Table of Contents
What Is Provider Credentialing?
Credentialing is the process of verifying a provider’s qualifications such as licensure, education, training, work history, and professional liability coverage so payers and networks can determine whether to add the provider to their participating panel. For most practices, credentialing is a prerequisite to being in-network and receiving contracted reimbursement rates.
Credentialing vs. Enrollment vs. Contracting
| Term | What it means | Typical output | Why it matters |
|---|---|---|---|
| Credentialing | Verification of provider qualifications and background | Approved credentials file | Required to join many payer networks |
| Enrollment | Registering the provider or group in a payer’s billing system | Payer ID or billing record | Needed to submit claims and receive payments |
| Contracting | Negotiating or accepting participation terms and reimbursement rates | Executed contract with effective date | Determines in-network status and reimbursement |
What You Need Before You Start
Common items payers request (varies by payer and specialty)
- National Provider Identifier (NPI) for the individual provider (Type 1) and for the organization (Type 2), as applicable
- Active state professional license(s) and any specialty certifications
- Malpractice/professional liability insurance declarations page
- Education and training history (schools, graduation dates, residencies/fellowships if applicable)
- Work history with month/year gaps explained
- Practice location(s), phone/fax, tax ID, W-9, and banking details for EFT (as required)
Tip: consistency prevents delays
Credentialing is detail-heavy. Small mismatches across forms (addresses, dates, provider names, licenses) are a common cause of returned applications and follow-up requests. Standardizing your “source of truth” profile reduces rework.
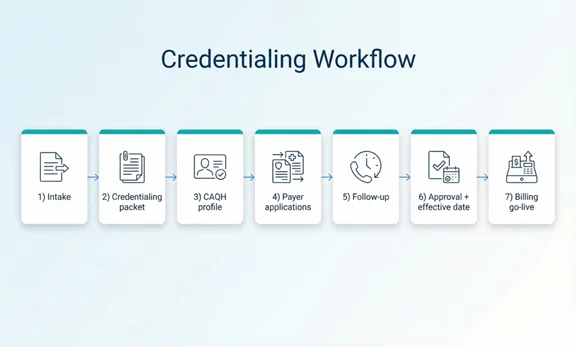
Step-by-Step Credentialing Process
- Intake and payer targeting: Confirm your service lines, locations, and which payers you want to join. Define the order of applications based on demand and payer requirements.
- Build a complete credentialing packet: Collect and validate licenses, liability coverage, education/training history, work history, and practice/business documents. Resolve gaps before submission.
- Create or update CAQH profile (when required): Many payers use CAQH as a centralized provider data source. Complete the profile, upload documents, and attest to accuracy.
- Submit payer enrollment/credentialing applications: Submit required payer applications and supporting documents. Track submission dates, reference numbers, and payer portals.
- Follow up and respond to payer requests: Credentialing often requires follow-up: missing forms, clarifications, and additional verifications. Fast responses shorten time-to-approval.
- Confirm approval and effective dates: Capture approval letters and effective dates. Ensure provider is loaded correctly in payer systems to avoid claim denials.
- Post-approval setup (billing readiness): Confirm how claims should be submitted, where remittances/ERAs are accessed, and whether EFT is active so payments flow correctly.
- Ongoing maintenance and re-credentialing: Keep profiles current (addresses, licenses, insurance). Track re-attestations, re-credentialing cycles, and Medicare revalidations to prevent disruptions.

CAQH ProView / Provider Data Portal: Setup + Maintenance
CAQH’s Provider Data Portal (formerly CAQH ProView) allows providers to enter their information once and share it with participating plans they authorize. Keeping your CAQH profile active and accurate helps reduce repeated paperwork across payers.
Re-attestation cadence
CAQH requires periodic re-attestation to confirm your information remains accurate. Set reminders and complete re-attestation on time to avoid profile lapse.
What to keep updated
- License renewals and board/specialty certifications (as applicable)
- Malpractice/professional liability policy renewals
- Practice locations, phone/fax, and billing addresses
- Hospital affiliations (if applicable) and work history updates
- Tax and banking information for EFT (when required by payers)
Medicare Enrollment and Revalidation Basics
If your practice bills Medicare, enrollment is commonly managed through the CMS Provider Enrollment, Chain, and Ownership System (PECOS) or via paper forms (for example, CMS-855 forms depending on provider type). Medicare also requires periodic revalidation to maintain billing privileges.
Common Medicare-related touchpoints
- NPI application/updates through the National Plan and Provider Enumeration System (NPPES)
- Enrollment applications (CMS-855 forms depending on provider/supplier type)
- Revalidation schedule monitoring and timely submission
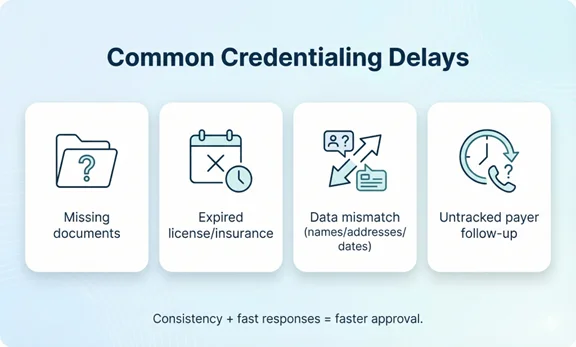
Common Delays (and How to Prevent Them)
Most common avoidable issues
- Incomplete or illegible document uploads (especially insurance and licenses)
- Inconsistent addresses, dates, or names across forms and CAQH
- Missing explanations for employment gaps
- Out-of-date CAQH profile (missed re-attestation)
- Not tracking payer follow-up requests or portal messages
Preventive checklist (quick)
| Before submission | After submission |
|---|---|
| Standardize provider demographics (name, addresses, contact) | Log submission date, payer reference number, and portal status |
| Verify licenses and insurance are current and readable | Follow up on payer requests within 24–48 hours |
| Confirm CAQH sections are complete and attested | Record approval and effective date; confirm provider is loaded |
| Maintain a single credentialing packet folder | Confirm claim submission and ERA/EFT setup for billing readiness |

KPIs to Track After You’re Credentialed
- Time-to-credential (days from intake to approval)
- Approval rate by payer (first-pass vs. resubmissions)
- Effective date accuracy (avoid backdated or missing effective dates)
- Initial claim acceptance rate (rejection/denial rate right after go-live)
- Re-credentialing compliance (on-time renewals and CAQH re-attestations)
Security, Privacy, and Compliance Notes
Credentialing involves sensitive personal and business documents. Use role-based access, least-privilege permissions, and secure file sharing. Maintain an audit trail for who accessed or changed provider records, especially when multiple staff members support credentialing.
How Claim N Billing Handles Credentialing
We run credentialing as a tracked workflow: build a complete packet, keep CAQH current, submit payer applications, follow up fast, and document approvals/effective dates so billing can go live smoothly.
What you get
- Credentialing intake + payer targeting plan
- CAQH setup, document upload, and re-attestation tracking
- Payer application submission + portal tracking
- Follow-up management and status updates
- Approval and effective date documentation
- Post-approval billing readiness checklist (claim submission + remittances)
Frequently Asked Questions
What is the difference between credentialing and enrollment?
Credentialing verifies provider qualifications; enrollment registers the provider/group in the payer system so you can bill and get paid.
What is CAQH and why do payers ask for it?
CAQH’s Provider Data Portal is a centralized repository where providers can store and share credentialing information with authorized plans.
How often do I need to re-attest CAQH?
CAQH requires re-attestation on a periodic cycle to confirm your profile remains accurate. Missing it can cause your profile to lapse.
How often do payers re-credential providers?
Many organizations follow a recurring re-credentialing cycle. Network standards commonly use a three-year cycle, but requirements can vary by payer and state.
How often does Medicare revalidate enrollment?
Medicare requires periodic revalidation to maintain billing privileges; in general, providers and suppliers revalidate every five years (with some supplier exceptions).
Do I need an NPI before credentialing?
In most cases, yes. The NPI is a standard identifier used in healthcare transactions and is commonly required on payer applications.
How long does credentialing take?
Timelines vary by payer and completeness of your application. A complete packet and fast responses to payer requests can shorten turnaround.
What documents are commonly needed?
Common items include licenses, liability insurance, education/training history, work history, practice addresses, and business/tax documents.
What causes credentialing delays most often?
Missing documents, inconsistent information across forms and CAQH, expired policies/licenses, and slow responses to payer follow-up.
What happens after approval?
Confirm effective dates, ensure the provider is loaded correctly, verify claim submission and remittance access, and set up EFT/ERA where needed.
Can you help with ongoing maintenance?
Yes. Maintenance includes CAQH re-attestation, license/insurance tracking, payer updates, and re-credentialing cycle management.
What do you need from our clinic to start?
Provider demographics, licenses, liability insurance, education/work history, practice details, tax/W-9 information, and your target payer list.
Ready to Get Credentialed Without Costly Delays?
Let’s walk through your current workflow and show you how we can support your practice.
Your billing should be as reliable as your care.
