Key Differences Between Hospital Billing vs Professional Billing

When a patient walks into a healthcare facility for the first time, whether it’s a large hospital or a small doctor’s office, billing is a complex process that unfolds in the background. However, it’s important to understand the differences between hospital billing vs professional billing. They reflect different ways in which providers are reimbursed for services. Differences between the two are important for clinic administrators, medical billing professionals, and patients trying to understand the U.S. healthcare system. This blog aims to demystify the principles behind the two with the help of practical examples to explain the different processes involved and the reasons behind them.
What Is Hospital Billing?
Hospital billing is synonymous with facility billing and is the charge for services rendered by a hospital or healthcare facility. Remember this as the charge for the ‘location’ where healthcare is provided. This also extends to hospital furnishings and all personnel on duty. Hospitalizations for surgery and visits to the emergency care area incur such expenses. These costs relate to the level of care you received when you were admitted.
To track the services provided, hospitals document the services using ICD-10 codes for diagnoses and then assign a DRG (Diagnosis-Related Group) code for the inpatient stay. These codes also define the reimbursement the hospital will receive from the payers, be it Medicare, Medicaid, or a private insurer. For instance, you were hospitalized for appendicitis, and the hospital sends a claim with ICD-10 code K35.80 (unspecified acute appendicitis) and a DRG code for grouping your treatment for reimbursement.
In hospital billing, the charge entry process records all hospital services such as laboratory tests, imaging, room charges, meals, and other services on a patient’s account. The billing team then submits these recorded items as a claim to a clearinghouse or payer for processing. Because hospitals handle thousands of claims each day, they rely on dedicated billing departments supported by advanced electronic health record (EHR) systems to manage the workload efficiently.
Picture yourself in the ER with a broken arm. You get billed for the X-ray, the ER room, and the attending nurse. These costs are incurred at the facility level and do not include the price for the doctor’s time who came to reset the arm.
What Is Professional Billing?
This type of billing covers services of specific health care professionals, i.e., physicians, doctors, and nurse practitioners and is unrelated to the facility. Professional billing is most common in outpatient scenarios, like a visit to a physician’s office or a specialty clinic.
Professional billing uses Current Procedural Terminology (CPT) codes for procedures done. For instance, a cardiologist billing for a performed EKG uses code 93000. These codes get paired with ICD-10 codes for medical necessity and approval from the payer.
Unlike hospital billing, which uses bundled payments, professional billing is much more detailed and focused on individual procedures. The billing staff of the physician practice sends the claim to the payer and to the clearing house for payer approval. This is most important for the financial viability of independent practitioners or physicians not affiliated with a hospital.
Consider the example of the skin biopsy. The professional bill for that includes the time the physician spends performing the biopsy and the time the physician spends analyzing the results. If the procedure occurs in a hospital-owned facility, a separate hospital bill might cover the exam room or the equipment cost.
Key Differences Between Hospital Billing vs Professional Billing

The differences between hospital billing vs professional billing affect claim submission and revenue cycle management (RCM). Let us look at these differences a little closer.
1. Scope of Services
For hospital billing, a hospital facility encompasses all resources, including:
- Room and board for inpatient services
- Diagnostic tests (e.g., MRIs, blood work)
- Medical supplies and equipment
- Support staff (nurses, technicians)
For professional billing, services by licensed providers include:
- Consultations
- Surgical procedures
- Diagnostic interpretations
- Follow-up visits
For example, during knee surgery, the hospital bill covers the operating room and the anesthesia equipment, while the professional bill covers the surgeon’s expertise.
2. Coding Systems
Hospitals use DRG codes for inpatient services, APC (Ambulatory Payment Classification) codes for outpatient services, and ICD-10 codes. These codes bundle services for standardized reimbursement.
All insurance companies have unique billing procedures that use the required documentation. Submitted bills can be broken down into line-by-line collections easily. For instance, a hospital may bill the ER visit using a single DRG code, while ER physicians submit CPT codes for their evaluations and procedures, and the count goes to the hospital’s total billing.
3. Reimbursement Models
Hospitals mainly process DRG and APS bundled payments for Medicare and Medicaid patients. This entails making a single fixed payment for a particular patient’s stay, regardless of all the services rendered.
Professional billing tends to operate on the fee-for-service model, meaning payment for each procedure and service rendered to a particular patient. This entails using precise codes since each CPT code must correlate with an ICD-10 code to show proof of medical necessity and avoid tighter scrutiny from payers.
4. Claim Submission Process
Claim submission is part of the billing process and can be quite tedious. For hospitals, it is a high volume. A patient’s stay can consist of dozens of charges. This is where documentation needs to be at a high standard for EHR systems.
Professional billing is more straightforward because it deals only with the services that one provider renders. In small practices, billing software or outsourced revenue cycle management can compensate for the absence of more sophisticated EHRs.
5. Inpatient vs Outpatient Focus
Hospital billing usually pertains to services where patients stay overnight or to more complex outpatient procedures being performed in a hospital. Professional billing is more common with outpatient services such as office visits or minor procedures done in clinics.
As an illustration, outpatient surgery at a hospital-owned surgical center could generate two bills: one as a hospital facility charge and another as a professional charge for the surgeon.
Why These Differences Matter
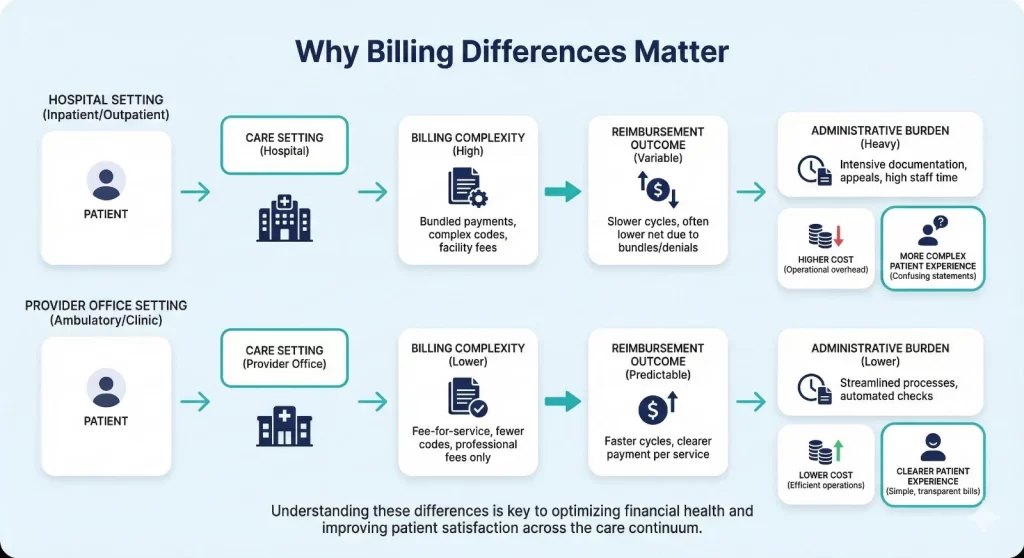
The distinction is extremely important for both patients and providers in the healthcare system. For providers, it defines revenue cycle management and negotiations with payers. Proper coding and timely filing of claims are needed to prevent claims rejections and keep a positive cash flow for the healthcare business. For patients, it explains the multiple bills they receive for one healthcare service a facility charge, a professional service charge, and individual charges for any radiology or laboratory tests performed. It helps explain any surprises they encounter while reviewing an insurance explanation of benefits.
Imagine Jane having a hospital colonoscopy and how the billing would go about.
Each hospital component includes the procedure room, the endoscopy equipment, and the nursing staff, and then a claim is submitted. Jane’s hospital’s facility claim receives an outpatient procedure APC code and an ICD-10 code Z12.11 for colorectal cancer screening, bundled to an outpatient payment claim for an outpatient procedure.
The claim for the colonoscopy also includes the paired ICD-10 code for the procedure and CPT code 45378 for professional billing. The insurance reimbursement follows the designated payment schedule.
Then Jane would receive two bills, one from a hospital for the facility costs and one for the hospital’s professional services. If both the hospital and gastroenterologist are in-network, her out-of-pocket costs would be lower; otherwise, she would have higher fees.
Best practices for handling and professional billing are different, and each faces differing challenges with medical claim processes.
With their own set of regulations, hospitals handle high claim volumes and complicated DRG reimbursement, where mistakes in DRG coding workflows expose and increase denial and audit risks. A 2023 American Hospital Association study revealed that payers deny 15% of hospital claims, prompting hospitals to resubmit and restore those denied claims.
Billing management is often underfunded in charge entry and denial follow-up, particularly in small practices. Romadano says, “The denial of a claim because of a faulty CPT-ICD-10 pairing can put a cash flow on hold.” A 2024 Medical Group Management Association report, as cited in Romadano, suggests that small practices lose nearly 10% of their revenue because of coding errors.
Claims clearinghouses improve the process by checking for errors before submission, which reduces denials. More sophisticated EHR systems ease coding by spotting missing documentation, such as ICD-10 codes. An EHR can, for example, notify a biller of a mismatched code, which will help avoid a rejection.
Payer requirements amplify these issues. Medicare and private payers ask for documentation of medical necessity, while hospitals deal with value-based care models, which tie reimbursement to outcomes. Professional billers contend with prior authorizations, which create lags in planned procedures and payments.
From the Patient Perspective and Communication
For patients, such systems can be opaque. A 2024 Kaiser Family Foundation study found that 45% of patients struggled to understand their medical bills, often because providers issued multiple charges for a single visit. Help patients avoid frustration by clarifying the difference between professional and facility charges through a billing FAQ on the patient portal.
Consider a scenario where a hospital bills a patient for an MRI and then the radiologist sends a separate bill for the interpretation. Explaining why both services are billed separately will foster understanding, promote trust, and minimize disagreements over the bill.
Strategies for Healthcare Providers Relating to Billing
Here are practical measures clinic administrators and billers can take to balance hospital and professional billing.
-
- Educate Your Staff: Having staff trained in billing coding for CPT, ICD-10, DRG, and APC will enhance proficiency. Studies claim that the coding/ billing training helped reverse a 20 percent hospital claim denial rate within a year, 2022 Invensis case study.
-
- Optimize your Billing Workflow: Automate charge captures in your EHR and billing systems and set automated claim submission processes. Automation removes unnecessary delays in payment and billing errors.
-
- Analyze Denied Claims: Investigate denied claims to research coding patterns that could be leading to claims denials. This is vital for managing the revenue.
-
- Provide Information: Provide a succinct explanation when patients are sent multiple bills. Information is most helpful when provided in a billing FAQ.
-
- Consider Outsourcing: Small practices have seen a 15 percent improvement in collections after outsourcing RCM, particularly for professional billing, 2023 HFMA report.
Conclusion
The variations in hospital billing and professional billing come from differences in scope, coding, and payment. With hospital billing, billing DRGs and APCs cover facility resources, while professional billing pertains to provider services and uses CPT codes for fee-for-service reimbursement. While both are part of the healthcare reimbursement ecosystem, they serve different functions.
Understanding these differences allows providers to optimize their processes for more efficient medical claims processing and improved fiscal results. These distinctions clarify billing, facilitating the insurance and payment processes for patients. Whether overseeing a hospital billing department or a smaller physician practice billing team, managing these complexities is crucial in a challenging healthcare revenue environment.
For expert support with hospital vs professional billing or revenue cycle management, contact Claim N Billing.com. Our certified specialists optimize claims and maximize reimbursements.
