Chiropractor Billing Services in California
Professional Billing Services for Chiropractors
Chiropractors help patients move better, feel better, and live better through adjustments, therapies, and personalized care plans. But the paperwork behind it all? Insurance verifications, detailed progress notes, CPT coding for manipulations, and navigating payer rules can pull you away from what you do best.
Most chiropractors we talk to say the same:
- I’m great at adjustments, but billing codes feel like a puzzle I don’t have time for
- Denials keep coming back because of ‘medical necessity’ issues
- I spend too many evenings chasing claims instead of prepping for tomorrow’s patients
- I need someone who gets the chiropractic world to handle this reliably
That’s where Claim N Billing steps in. We specialize in billing for solo practitioners, multi-doctor clinics, and wellness centers ensuring your claims are accurate, compliant, and reimbursed without the hassle.
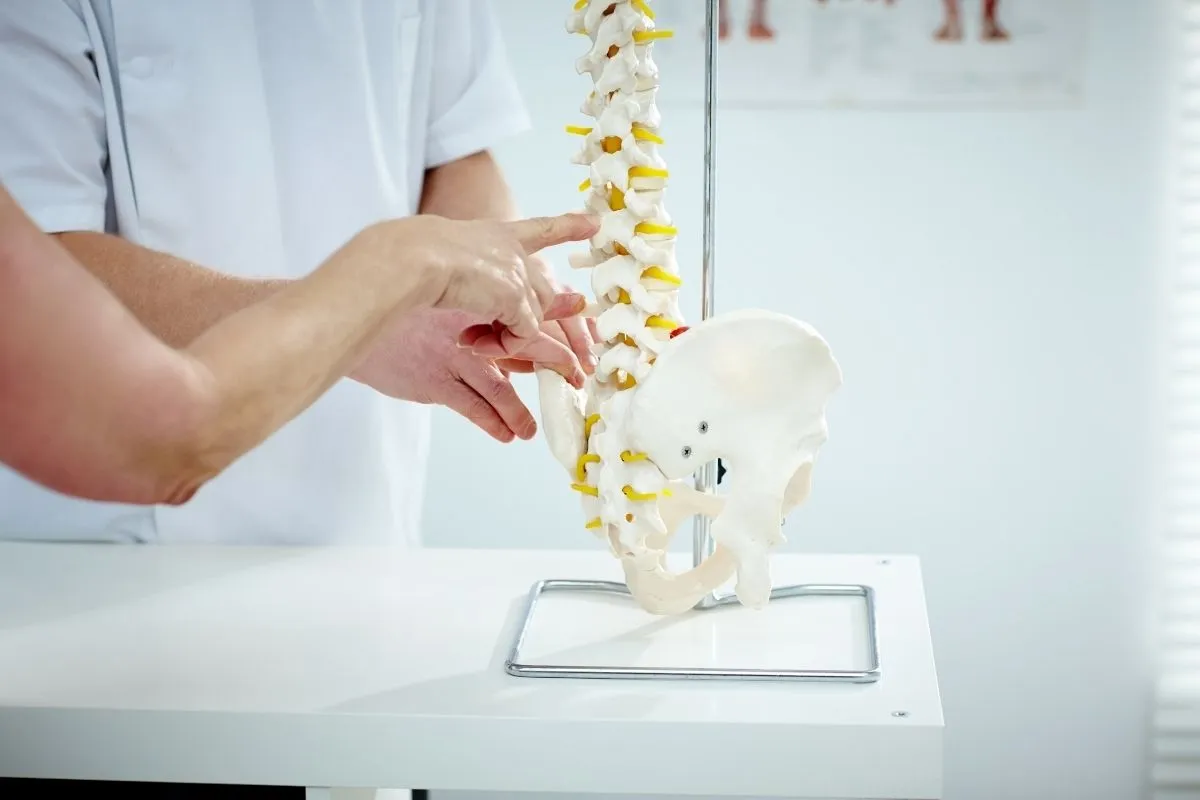
What Is Chiropractor Billing?
Chiropractor billing covers submitting claims for spinal manipulations, extremity adjustments, evaluations, therapies like ultrasound or electrical stimulation, and follow-up visits using specific CPT codes and detailed documentation to prove medical necessity.
It gets tricky because:
- Manipulation codes (98940–98943) require precise session notes on areas treated and patient response
- Payers demand strict proof of medical necessity to avoid denials
- Auto accident or workers’ comp claims add layers of coordination and forms
- Coverage for adjunct therapies varies widely by insurer
We handle the details so your reimbursements come through smoothly and you stay focused on patient adjustments.

Why Chiropractors Choose Claim N Billing
From private practices to those billing auto insurers or Medi-Cal, we understand the unique flow of chiropractic revenue and we make it work for you.
- Specialized in chiropractic CPT coding and documentation standards
- Full support for credentialing with major payers and Medi-Cal enrollment
- We manage claims, follow-ups, and appeals tailored to manipulation services
- Clear, monthly reports on your cash flow and denial trends
- Dedicated specialist who knows chiropractic workflows inside out
- Compliant with HIPAA and California-specific rules for seamless operations
We’re not just billers we’re partners who’ve walked in your shoes, simplifying the business side so you can keep adjusting lives.
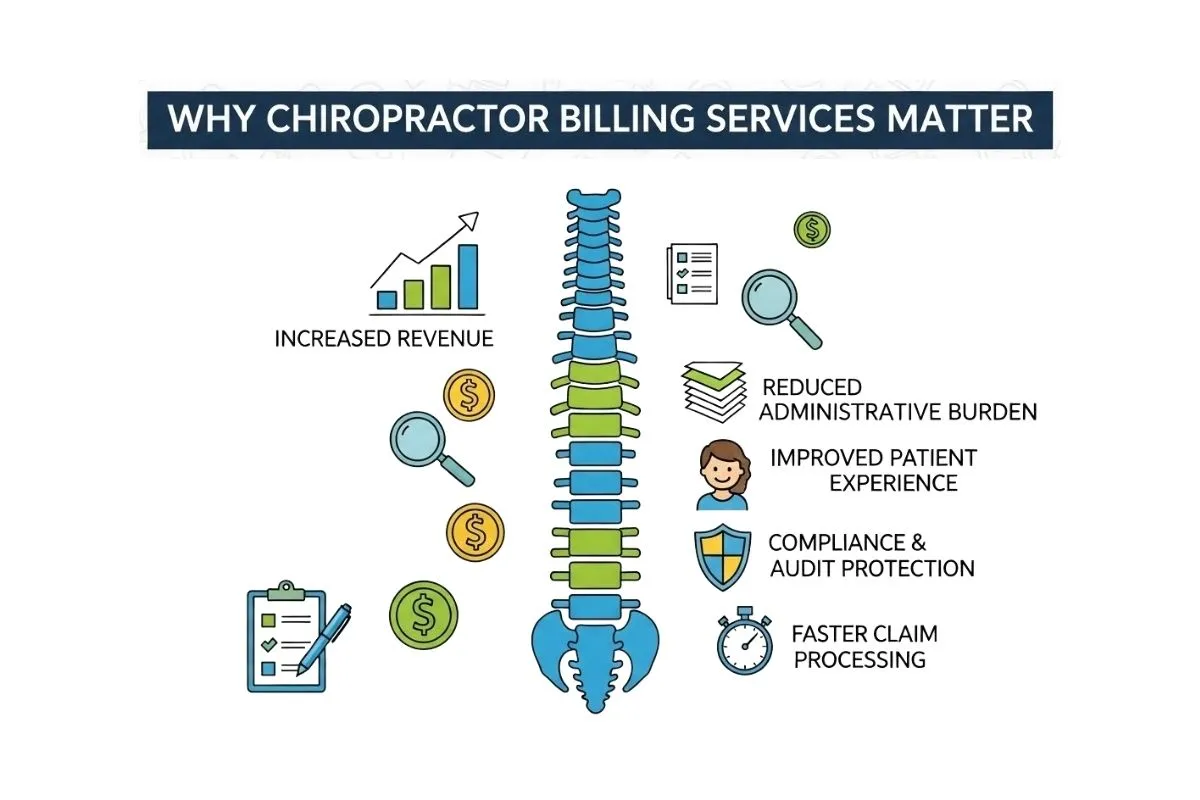
Why Chiropractor Billing Services Matter
Chiropractors dedicate their days to hands-on healing, but billing roadblocks can disrupt your practice and income. Here are the top challenges we hear:
-
Coding errors lead to denials
Manipulation codes need exact documentation—one slip, and claims bounce back. -
Medical necessity documentation is exhaustive
Payers scrutinize every note, turning simple adjustments into hours of justification. -
Auto and workers’ comp claims drag on
Coordinating with adjusters and third parties delays payments for months. -
Admin time steals from patient care
You lose 5–8 hours weekly on verifications, submissions, and appeals. -
Unclear revenue tracking stalls growth
Without insights into what’s paid or pending, it’s hard to plan expansions or hire help.
We tackle every one of these, freeing you to focus on what matters most your patients.
The Services We Provide

Claim Submission & Follow-Up
This is where your revenue actually starts moving.
Once care is provided, claims have to be created correctly, submitted on time, and actively followed, not sent out and forgotten. That’s the work we handle every day.
We take responsibility for turning your visits into clean, accurate claims and staying on top of them until there’s a clear response from the payer.
What this includes:
- Accurate claim creation and submission
- Verification that payer and provider details are correct before submission
- Timely filing to avoid avoidable denials
- Ongoing claim tracking after submission
- Follow-up with payers until claims are processed
- Correction and resubmission when issues arise

Denials Management & Appeals
This is where most revenue is quietly lost — and where we’re the most hands-on.
We don’t submit claims and move on. Every claim is tracked, monitored, and followed until there’s a clear outcome.
How we protect your revenue:
- Accurate claim creation and submission
- Correct CPT, ICD, and modifier usage
- Daily tracking and payer follow-up
- ERA/EOB posting and reconciliation
- Secondary and corrected claims handling
- Appeals written and pursued when payment is owed

Prior Authorizations
Most practices don’t realize how much revenue they lose from missing or incorrect authorizations, until it’s too late.
We step in early to prevent those losses.
What we handle:
- Identifying services that require authorization
- Catching recurring denial patterns tied to auth issues
- Submitting and following up on authorizations
- Managing appeal documentation when needed
- Rebilling and recovery when claims are incorrectly denied

Credentialing
Credentialing isn’t just paperwork — it directly impacts whether you get paid at all.
We handle credentialing with the same attention we give claims, because front-end mistakes cause most downstream denials.
Our role includes:
- Provider enrollment and payer setup
- Ongoing credential maintenance
- Eligibility and payer readiness checks
- Ensuring provider records stay current and compliant

Appointment Setting
You shouldn’t have to guess how your practice is performing, or where your money stands.
We provide clear visibility into what’s happening, what’s pending, and what needs attention.
You receive insight into:
- Claims submitted vs. claims paid
- Denial trends and payer behavior
- Aging and outstanding balances
- Revenue patterns and cash-flow timing
- Practical recommendations based on real data

Monthly Financial Reporting
Billing works best when the entire workflow is connected.
We align scheduling, documentation, and claims so nothing falls through the cracks.
What this supports:
- Fewer missed or delayed charges
- Cleaner documentation
- Faster claim turnaround
- A more predictable billing pipeline

Payment Posting & Reconciliation
Accurate payment posting matters just as much as claim submission.
We make sure payments, adjustments, and write-offs are correctly reflected, so your numbers tell the truth.
This includes:
- ERA and EOB posting
- Payment reconciliation
- Coding and documentation reviews
- Audit readiness support
- Compliance guidance for telehealth, E/M, and specialty rules
Our services are designed to support practices at different stages, whether you need help in one area or across your entire billing workflow.
01
Consultation & Account Setup
We dive into your practice flow, codes, and current challenges to create your custom billing setup.
02
Insurance Verification
We confirm patient coverage and chiropractic benefits prior to services.
03
Claim Submission
We prepare and file precise claims with full documentation for manipulations and therapies.
04
Payment Posting
We apply payments, resolve discrepancies, and track outstanding balances.
05
Reporting & Ongoing Support
Monthly breakdowns of your revenue, plus tips to reduce future denials.
Chiropractor Insurance & Medi-Cal Expertise
Chiropractic billing involves navigating strict payer guidelines, from Medicare’s manipulation limits to California’s Medi-Cal chiropractic benefits. Our team keeps you ahead:
- Medi-Cal chiropractic enrollment and coverage rules
- Medicare documentation for medical necessity
- Auto insurer requirements for personal injury claims
- Approved CPT/HCPCS codes for adjustments and modalities
- State-specific compliance for telehealth evals (when allowed)
- Appeal strategies for common denials like frequency caps
We ensure every claim aligns with these rules, maximizing your approvals and reimbursements.
Client Success Stories
Frequently Asked Questions
Ready to Streamline Chiropractic Billing With Confidence?
Let’s review your setup and show you how we can ease the load on your practice.
Your adjustments deserve billing that aligns just as well.
