Medical Billing for Small to Medium Clinics in California
Professional Billing Services for Small To Medium Clinics
Running a small to medium clinic means juggling patient care across multiple providers, specialties, and daily appointments while keeping the lights on through consistent reimbursements. But scaling up often uncovers hidden billing hurdles: coordinating claims across teams, staying compliant with evolving payer rules, and tracking revenue without losing sight of growth opportunities.
Most clinic owners and administrators share these frustrations:
- With more providers, our claims volume exploded, but so did the denials
- I’m constantly verifying insurance for different specialties it’s exhausting
- Paperwork is pulling our staff away from patients, not helping them
- We need reliable billing that grows with us, without the big-firm prices
Claim N Billing gets it we’ve been there, starting from our own non-emergency medical transport roots and building expertise in supporting practices just like yours. We tailor billing for multi-provider clinics with 2–20 staff, from primary care to integrated specialty groups, so you can focus on expanding care, not chasing payments.

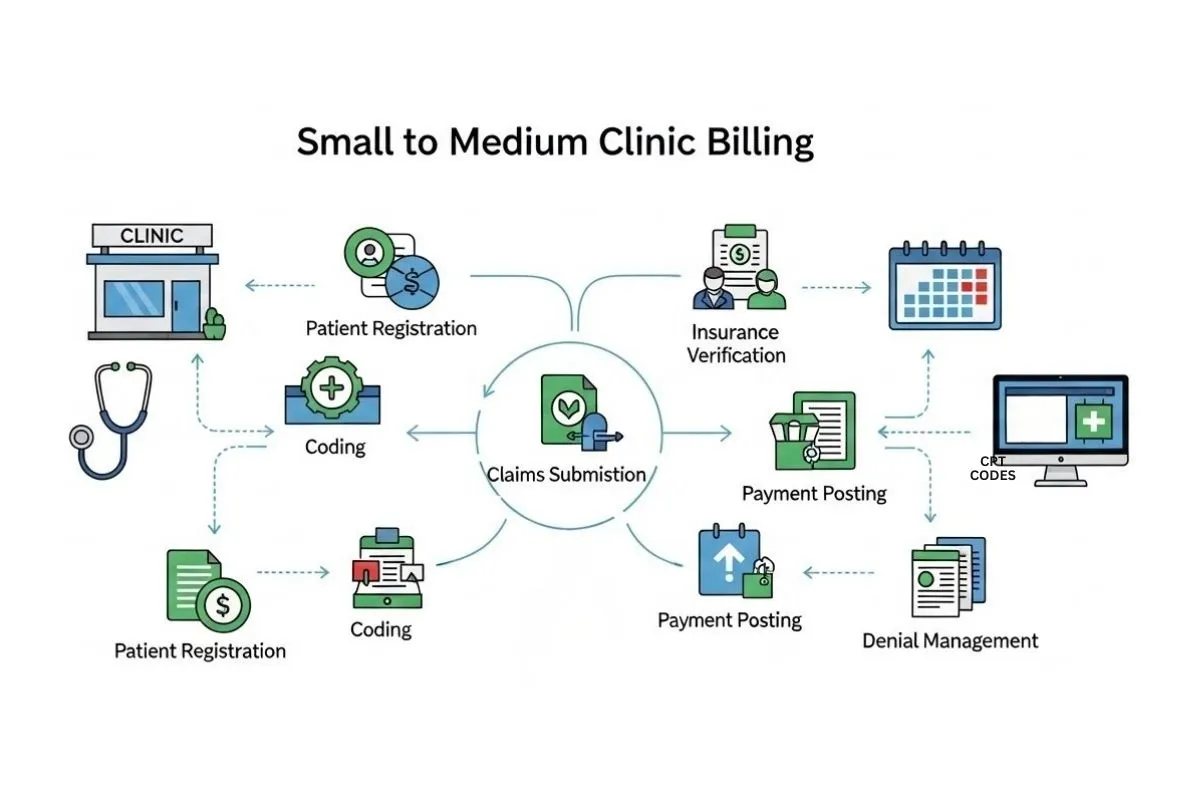
What Is Small to Medium Clinic Billing?
Small to medium clinic billing involves managing claims for a range of services routine visits, diagnostics, procedures, and specialist consultations across multiple providers, using coordinated CPT codes, eligibility checks, and detailed documentation to meet diverse payer requirements.
It’s especially demanding because:
- Claims must align across providers and specialties, with shared patient records
- Volume grows quickly, leading to errors in high-throughput environments
- Payers like Medicare and commercial insurers have varying rules for group practices
- Revenue cycle gaps can compound, delaying cash flow for the whole clinic
We streamline it all, integrating your workflows to ensure accurate submissions and faster resolutions, so your clinic runs like a well-oiled team.

Why Small to Medium Clinics Choose Claim N Billing
We know the pressures of growing a practice without the resources of a large hospital system. Our approach fits seamlessly into your operations, handling everything from credentialing to reporting with the personal touch of a dedicated partner.
- Expertise in multi-provider billing and cross-specialty coordination
- Customized credentialing for groups, including Medicare, Medi-Cal, and commercial panels
- End-to-end claims management, from verification to appeals, scaled to your volume
- Transparent monthly dashboards tracking clinic-wide revenue and bottlenecks
- A single point of contact who learns your unique setup and adapts as you grow
- Full HIPAA compliance with secure systems built for collaborative environments
We’re the billing ally that’s been in the trenches with small practices, helping you turn administrative chaos into sustainable growth.
Why Small to Medium Clinic Billing Services Matter
For small to medium clinics, billing isn’t just paperwork it’s the backbone of stability and expansion. Yet, as your team grows, so do the cracks in the system. Common hurdles include:
-
Fragmented claims across providers
Inconsistent coding or notes lead to widespread denials and rework. -
Eligibility surprises disrupt scheduling
Unverified coverage for new patients causes last-minute cancellations and lost slots. -
Scaling admin without scaling staff
Billing tasks multiply, eating into time for hiring or training. -
Cash flow dips from delayed payments
Group claims get stuck in review, straining budgets for supplies or payroll. -
Lack of visibility hampers decisions
Without clear metrics, it’s tough to spot trends or justify investments in your practice.
We address these head-on, creating a unified system that supports your clinic’s momentum and lets your provider’s shine.

The Services We Provide

Claim Submission & Follow-Up
This is where your revenue actually starts moving.
Once care is provided, claims have to be created correctly, submitted on time, and actively followed, not sent out and forgotten. That’s the work we handle every day.
We take responsibility for turning your visits into clean, accurate claims and staying on top of them until there’s a clear response from the payer.
What this includes:
- Accurate claim creation and submission
- Verification that payer and provider details are correct before submission
- Timely filing to avoid avoidable denials
- Ongoing claim tracking after submission
- Follow-up with payers until claims are processed
- Correction and resubmission when issues arise

Denials Management & Appeals
This is where most revenue is quietly lost — and where we’re the most hands-on.
We don’t submit claims and move on. Every claim is tracked, monitored, and followed until there’s a clear outcome.
How we protect your revenue:
- Accurate claim creation and submission
- Correct CPT, ICD, and modifier usage
- Daily tracking and payer follow-up
- ERA/EOB posting and reconciliation
- Secondary and corrected claims handling
- Appeals written and pursued when payment is owed

Prior Authorizations
Most practices don’t realize how much revenue they lose from missing or incorrect authorizations, until it’s too late.
We step in early to prevent those losses.
What we handle:
- Identifying services that require authorization
- Catching recurring denial patterns tied to auth issues
- Submitting and following up on authorizations
- Managing appeal documentation when needed
- Rebilling and recovery when claims are incorrectly denied

Credentialing
Credentialing isn’t just paperwork — it directly impacts whether you get paid at all.
We handle credentialing with the same attention we give claims, because front-end mistakes cause most downstream denials.
Our role includes:
- Provider enrollment and payer setup
- Ongoing credential maintenance
- Eligibility and payer readiness checks
- Ensuring provider records stay current and compliant

Appointment Setting
You shouldn’t have to guess how your practice is performing, or where your money stands.
We provide clear visibility into what’s happening, what’s pending, and what needs attention.
You receive insight into:
- Claims submitted vs. claims paid
- Denial trends and payer behavior
- Aging and outstanding balances
- Revenue patterns and cash-flow timing
- Practical recommendations based on real data

Monthly Financial Reporting
Billing works best when the entire workflow is connected.
We align scheduling, documentation, and claims so nothing falls through the cracks.
What this supports:
- Fewer missed or delayed charges
- Cleaner documentation
- Faster claim turnaround
- A more predictable billing pipeline

Payment Posting & Reconciliation
Accurate payment posting matters just as much as claim submission.
We make sure payments, adjustments, and write-offs are correctly reflected, so your numbers tell the truth.
This includes:
- ERA and EOB posting
- Payment reconciliation
- Coding and documentation reviews
- Audit readiness support
- Compliance guidance for telehealth, E/M, and specialty rules
Our services are designed to support practices at different stages, whether you need help in one area or across your entire billing workflow.
01
Consultation & Account Setup
We map your providers, specialties, and current systems to build a tailored billing framework.
02
Insurance Verification
Proactive checks for all incoming patients, coordinated across your schedule.
03
Claim Submission
Consolidated filing with full documentation, routed through your group’s payer mix.
04
Payment Posting
Accurate allocation to providers and services, with alerts for discrepancies.
05
Reporting & Ongoing Support
Detailed monthly reviews with actionable insights to refine your revenue cycle.
Small to Medium Clinic Insurance & Medi-Cal Expertise
Billing for small to medium clinics means mastering a patchwork of policies, from Medicare’s group billing rules to California’s Medi-Cal expansions for community practices. We stay current so you don’t have to:
- Medi-Cal group enrollment and reimbursement guidelines for multi-provider setups
- Medicare compliance for shared services and incident-to billing
- Commercial payer negotiations for network participation and fee schedules
- Specialty-specific CPT updates and modifiers for integrated care
- State rules on telehealth groups and virtual coordination of care
- Strategies for appeals in high-volume denials, like documentation shortfalls
Every step ensures your claims are group-ready, compliant, and optimized for your clinic’s scale.
Client Success Stories
Frequently Asked Questions
Ready to Simplify Billing for Your Growing Clinic?
Let’s assess your current setup and map out a plan that supports your team’s growth.
Reliable revenue lets your clinic focus on what it does best caring for your community
