Claim Submissions & Follow-Up Services
What is claim submission and follow-up in medical billing?
Claim submission and follow-up is the workflow that takes a clinical charge from “ready to bill” to “paid and closed.” It includes cleaning and submitting claims (often via EDI), monitoring acknowledgments and payer acceptance, checking claim status, fixing rejections, resolving denials, appealing when appropriate, and resubmitting within payer deadlines so revenue doesn’t get stuck in A/R.

Table of Contents
What Are claim submission and follow-up Services?
Claim submission services focus on preparing and sending claims in a clean, payer-acceptable format. Follow-up services ensure those claims are received, processed, and paid by actively monitoring acknowledgments, claim status, and payer actions.
What’s included
- Claim scrubbing and validation (demographics, payer info, codes, modifiers, required fields)
- Electronic claim submission (clearinghouse or direct payer connections)
- Acknowledgment tracking and rejection correction
- Claim status monitoring and follow-up (batch or real-time methods depending on connectivity)
- Denial routing (correct, resubmit, appeal) with documentation tracking
- Underpayment flags and payer follow-up when paid amounts don’t align with expected amounts
- Patient responsibility workflow alignment (when applicable)
Claim Submission vs. Denial Management vs. A/R Follow-Up
| Workflow | Primary goal | Typical work items | Outcome |
|---|---|---|---|
| Claim submission | Get claims accepted cleanly | Scrub, submit, correct rejections | Accepted claims in payer system |
| Denial management | Fix denials and get paid | Correct/resubmit, appeal, provide docs | Denials resolved and paid/closed |
| A/R follow-up | Move unpaid balances forward | Status checks, payer calls/portals, escalation | Faster payment and cleaner aging |
How Electronic claim submission Works (EDI Overview)
Many payers accept professional healthcare claims submitted using the CMS-1500 claim form, which is the standard paper form used by physicians and other non-institutional providers. The CMS-1500 captures essential patient demographics, provider information, diagnosis codes (ICD-10-CM), procedure codes (CPT/HCPCS), modifiers, and charges required for claim adjudication. While some claims are submitted electronically, the CMS-1500 format remains widely used for paper submissions and as the structural basis for professional claim data.
Where the clearinghouse fits
A clearinghouse can apply front-end edits, route claims to different payers, and return reports/acknowledgments. Even with automation, exceptions still require disciplined follow-up to prevent aging drift.
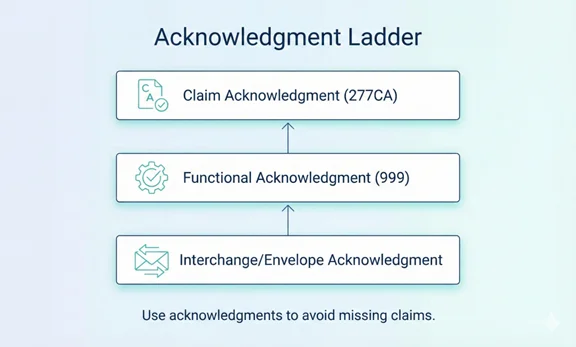
Acknowledgments: How to Avoid the "Black Hole"
A claim can fail at multiple points: file-level structure errors, claim-level rejections, or payer processing delays. Acknowledgment tracking provides proof of receipt and identifies where to fix issues fast.
Common acknowledgment layers (simplified)
- Interchange/Envelope acknowledgment (structure/transport confirmation)
- Functional acknowledgment (999) (confirms the file’s transaction sets were accepted for processing)
- Claim acknowledgment (277CA) (confirms which claims inside the file were accepted or rejected at the front-end)
Step-by-Step Claim Submission Workflow
- Charge review and readiness: Confirm required documentation, correct payer, member ID, dates of service, and rendering/billing provider information.
- Coding and data validation: Validate diagnosis/procedure codes, modifiers, place of service, units, and any payer-specific requirements.
- Claim scrubbing: Run edits to catch missing/invalid fields, formatting errors, and common payer rules before submission.
- Submit claims (EDI or paper, as required): Submit electronically where possible. Track batch IDs and submission timestamps.
- Monitor acknowledgments and correct rejections: Review acknowledgments on a fixed schedule. Correct errors and resubmit the same day when possible.
- Confirm payer acceptance and log payer claim IDs: Once accepted, capture payer claim IDs/control numbers for future status checks and follow-up.

Follow-Up Workflow: Claim Status + Next Actions
How status is checked
- Payer portals (manual review with notes)
- Clearinghouse status reports and dashboards
- EDI claim status inquiry/response in batch or real-time (depending on setup)
- Payer phone follow-up and escalation when needed
Status-to-action mapping (example)
| Status | What it usually means | Next action |
|---|---|---|
| Not on file | Payer has no record of claim | Verify acknowledgments, resubmit, confirm correct payer/receiver ID |
| Pending | In process / awaiting review | Check for missing info requests; set next follow-up date |
| Denied | Claim processed but not payable as submitted | Route to denial worklist: correct/resubmit or appeal |
| Paid | Remittance issued | Post payments/adjustments; check for underpayments |
| Requested documentation | Payer needs supporting info | Send requested docs quickly; confirm receipt |
Common Rejections And Denials How to Avoid the "Black Hole"
Rejections
Rejections usually mean the claim did not pass front-end edits (formatting or required-field rules). Fix the specific error, resubmit, and confirm a new acknowledgment.
Denials
Denials occur after the payer processes the claim and decides it’s not payable as submitted. Group denials into root-cause categories so prevention improves over time.
High-impact denial categories to track
- Eligibility/coverage issues
- Authorization/referral requirements
- Coding/documentation issues
- Timely filing
- Duplicate/bundling/coordination of benefits
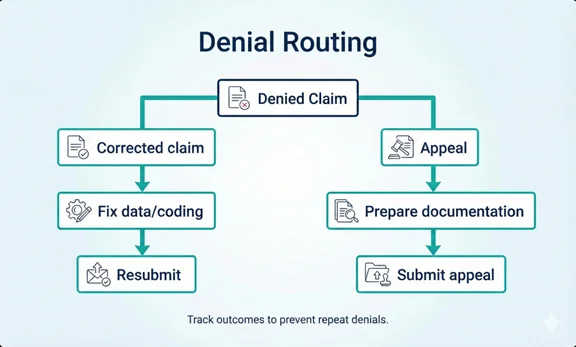
Appeals and Corrected Claims
A strong follow-up program uses clear rules: which denials require correction and resubmission, which require an appeal with documentation, and which are not viable based on plan policies.
Timely Filing and Resubmission Deadlines
Timely filing limits vary by payer, plan, and claim type. Build internal submission targets earlier than payer limits and track corrected claims and appeals separately.
KPIs to Track (Weekly/Monthly)
Weekly KPIs
- First-pass acceptance rate
- Rejection rate and top rejection reasons
- Denial worklist volume + aging
- Claims with “no status found” (potential black-hole risk)
Monthly KPIs
- Denial rate by payer and by category
- Appeal win rate (when tracked)
- A/R aging distribution by payer (trend)
- Resubmission/appeal turnaround time
Security, Privacy, and Compliance Notes
Claim follow-up involves sensitive patient and financial information. Use role-based access, least-privilege permissions, secure file sharing, and audit trails.
Claim Submissions & Follow-Up Cadence Checklist
We run claim submission and follow-up as a controlled workflow: clean submission, acknowledgment tracking, proactive status checks, and fast denial resolution. The goal is fewer preventable denials, faster payments, and a cleaner A/R aging profile.
What you get
- Claim scrubbing and clean submission process
- Acknowledgment monitoring and rapid rejection correction (where possible)
- Claim status follow-up cadence with documented outcomes
- Denial routing: correct/resubmit vs. appeal rules
- Escalation for high-dollar or aging claims
- Monthly trend reporting on rejections/denials and prevention recommendations

Frequently Asked Questions
What is the difference between a rejection and a denial?
A rejection usually means the claim failed front-end edits and wasn’t accepted into the payer processing system; a denial means the payer processed the claim and determined it’s not payable as submitted.
What is a 999 acknowledgment?
A 999 is a functional acknowledgment used in EDI to confirm whether transaction sets were accepted for processing at a standards/structure level.
What is a 277CA?
A 277CA is a claim acknowledgment that can provide claim-level acceptance or rejection details for claims contained in an 837 submission.
How do you check claim status electronically?
Many payers support a claim status inquiry/response process (often referenced as 276/277) in batch or real-time mode depending on connectivity.
What does “timely filing” mean?
Timely filing is the payer’s deadline for submitting an original claim or a corrected claim. Limits vary by payer and plan.
How do acknowledgments reduce revenue loss?
Acknowledgments prove whether a claim was received and identify rejections early, preventing claims from aging unnoticed.
Do you handle corrected claims and resubmissions?
Yes. Corrected claims and resubmissions are tracked so they stay within payer requirements.
What do you need from a clinic to start?
Access to billing/clearinghouse reports (as applicable), payer portal details, and your preferred reporting format.
Ready to Submit Claims Right and Get Faster Responses?
Let’s walk through your current workflow and show you how we can support your practice.
Your billing should be as reliable as your care.
