Payment Processing & Reconciliation Services
What is Payment Processing And Reconciliation in medical billing?
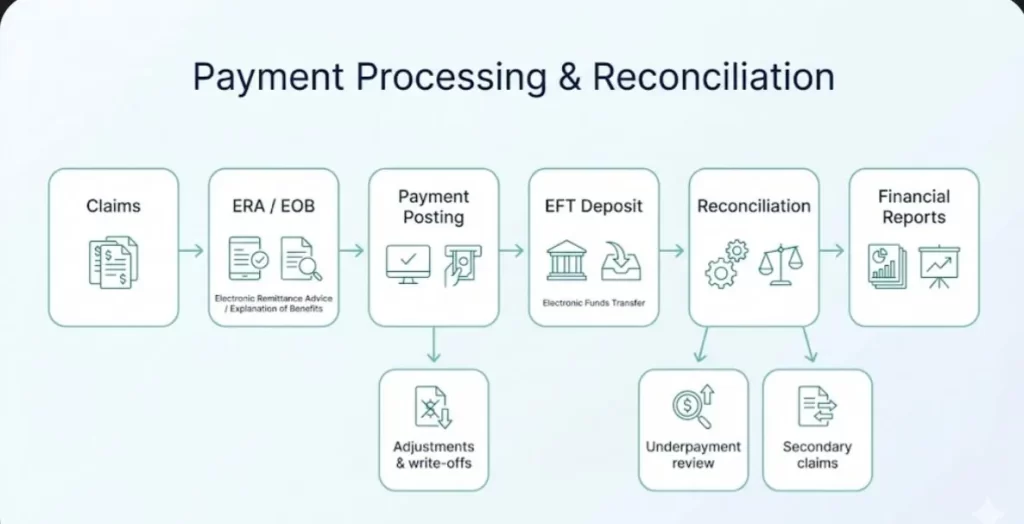
Payment processing and reconciliation is the back-end workflow that turns payer payments into accurate patient account balances and clean financial reporting. It includes posting payments from ERAs/EOBs, applying contractual adjustments, matching payments to bank deposits (EFT), identifying underpayments, triggering secondary claims when applicable, and ensuring your accounts receivable (A/R) reflects what is truly collectible.

Table of Contents
What Are Payment Processing & Reconciliation Services?
Payment processing and reconciliation services help practices accurately post payer and patient payments, reduce balance mistakes, and keep reports aligned with what actually hits the bank. In healthcare, this often revolves around Electronic Remittance Advice (ERA/835) files, paper remittances (EOBs), and Electronic Funds Transfer (EFT) deposits.
What’s included
- ERA/EOB payment posting (insurance payments and patient responsibility)
- Contractual adjustments and write-offs based on payer contracts and plan rules
- EFT-to-ERA matching (reassociation) so deposits match claim payments
- Denial and partial-payment handling (corrections, resubmissions, and appeal tracking)
- Underpayment identification and follow-up (allowed amount vs. paid amount review)
- Secondary claims and coordination of benefits (when applicable)
- Month-end reconciliation (deposit totals, posting totals, and A/R aging alignment)
- Clean reporting: payments, adjustments, refunds, and unapplied balances
Why Reconciliation Matters for Small Practices and Clinics
Posting is not just data entry. If payments are posted incorrectly or deposits are not reconciled, financial reports become unreliable, patient balances may be wrong, and A/R can look inflated. A consistent reconciliation process keeps cash flow predictable and prevents revenue leakage.
Common revenue leaks reconciliation prevents
- Underpayments that never get flagged for follow-up
- Duplicate postings or missed payments that distort patient balances
- Unapplied payments sitting in suspense (not linked to claims)
- Incorrect adjustments that hide real denials or create false write-offs
- Refund mistakes that cause compliance and patient experience issues

Payment Posting vs. Reconciliation (What’s the Difference?)
| Activity | What it does | Example output |
|---|---|---|
| Payment posting | Applies payer and patient payments to the correct claims and balances | Paid amounts and adjustments recorded on each claim |
| Reconciliation | Confirms posted totals match deposits and remittances, and flags discrepancies | Deposit-to-posting match with variance list |
| Underpayment review | Compares expected versus paid amounts and routes items for follow-up | Underpayment worklist and appeal tracking |
Setup Requirements: ERA/EFT, Payer Portals, and Reassociation
ERA (835) and EFT enrollment
To streamline posting and reconciliation, many practices enroll in ERA and EFT with payers. ERAs provide the electronic remittance details for each claim payment, and EFT provides the electronic deposit.
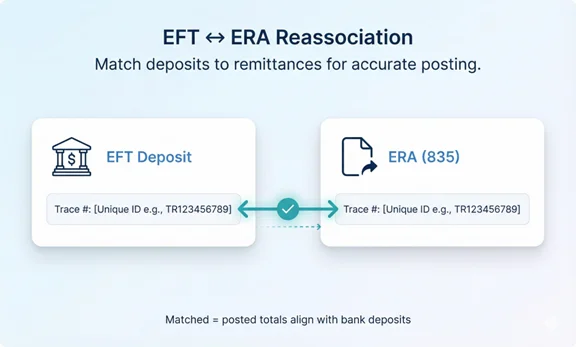
Reassociation: matching EFT deposits to ERAs
Reassociation is the process of matching the payer’s deposit to the correct ERA, so posting and bank reconciliation stay aligned. A consistent reassociation process reduces suspense balances and prevents missed payments.
Data you should standardize
- Payer names and plan IDs (so reports group correctly)
- Adjustment reason mapping (denials, reductions, patient responsibility)
- Write-off rules and approval permissions
- Refund workflow and documentation standards
Step-by-Step Payment Processing Workflow
- Retrieve the remittance (ERA/EOB) and payment: Download ERAs from your clearinghouse/payer portal and confirm EFT deposits. If you receive paper EOBs, scan and log them into a posting queue.
- Validate the remittance structure and identifiers: Confirm payer, provider identifiers, and trace/reference numbers so each payment can be matched and posted correctly.
- Post payments and apply adjustments: Post paid amounts, patient responsibility, and contractual adjustments consistently. Flag denials and partial payments for worklists.
- Handle denials, reductions, and missing information: Correct, resubmit, or appeal based on the reason codes and plan rules. Track outcomes so you can reduce repeat denials.
- Trigger secondary claims when applicable: If there is secondary coverage, submit secondary claims with the primary payer’s adjudication information.
- Reconcile deposits to postings (daily/weekly): Match EFT totals to posted totals and investigate variances such as missing ERAs, offsets, recoupments, or posting errors.
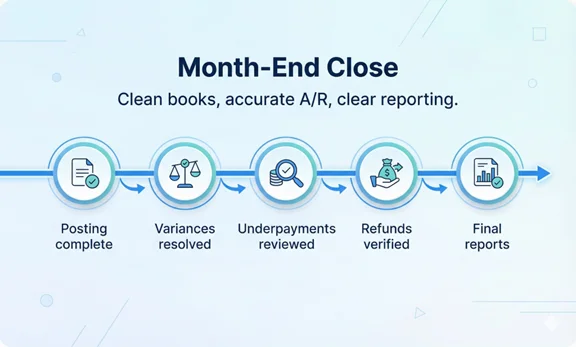
- Close the month with clean reporting: Confirm totals for payments, adjustments, refunds, and unapplied balances. Review A/R aging and fix outliers.

Common Issues That Cause Balance Errors
Partial payments and alternative benefits
Many plans pay less than expected due to policy limitations, bundling, alternative benefits, or coverage rules. A good process flags these as reductions vs. true denials, so you can decide whether to appeal or adjust patient responsibility.
Offsets, recoupments, and takebacks
Some deposits are reduced due to offsets/recoupments. These must be logged and reconciled so the remittance and the bank deposit align.
Unapplied payments and duplicate postings
Unapplied payments create false A/R and confuse patient balances. Duplicate postings can cause refunds and compliance headaches. A reconciliation checklist helps catch both quickly.
KPIs to Monitor (Weekly and Monthly)
Weekly
- Unapplied cash count and total dollar amount
- Denial/partial payment worklist volume and aging
- Deposit-to-posting variance (should trend toward zero)
- Underpayment queue size and resolution rate
Monthly
- A/R days and aging by payer (0–30, 31–60, 61–90, 90+)
- Write-off totals by reason (contractual vs. bad debt vs. courtesy)
- Refund counts and root causes (duplicate, over-collections, eligibility issues)
- Collections-to-charges ratio (trend, not one-off spikes)

Security, Privacy, and Compliance Considerations
Payment processing touches both financial data and, often, protected health information (PHI). Use secure access controls, least-privilege permissions, audit trails, and documented approval steps for write-offs and refunds.
Healthcare payment standards (ERA/EFT)
In the U.S., ERA (835) and EFT are standard healthcare transactions used to communicate payment and remittance details and deposit funds. Operating rules exist to improve consistency across payers and providers.
Card payments (if you accept credit/debit cards)
If your clinic processes card payments, use PCI DSS-aligned payment systems and avoid storing sensitive card data unnecessarily. Work with reputable processors and follow their compliance guidance.
Pricing Models and Timelines
Common pricing approaches
- Per-ERA / per-remittance volume pricing
- Percentage of collections (less common for posting-only)
- Monthly retainer for posting + reconciliation + reporting
What impacts cost the most
- Claim volume and payer mix
- How many payers require manual work vs. ERA automation
- Complexity: recoupments, frequent denials/appeals, multiple locations
- Quality of your current setup (clean mapping and workflows reduce time)
How Claim N Billing Handles Payment Processing
We treat payment processing as a control system: accurate posting, consistent adjustment rules, and reconciliation that keeps reporting aligned with cash. Our goal is fewer balance surprises, clearer A/R, and faster resolution of denials and underpayments.
What you get
- Payment posting (ERA/EOB) with consistent adjustment mapping
- Deposit matching and variance investigation
- Underpayment review and follow-up tracking
- Denial routing (correct/resubmit/appeal) and reporting
- Monthly close reporting: payments, adjustments, refunds, unapplied balances
Frequently Asked Questions
What is an ERA in medical billing?
An ERA (Electronic Remittance Advice) is the electronic version of a remittance that explains how a payer processed and paid a claim, including adjustments and patient responsibility.
What is the 835 transaction?
The 835 is the standard electronic transaction format commonly used to send ERA payment and remittance details from payers to providers or their billing partners.
What is the difference between ERA and EOB?
An EOB is often a paper or portal-view explanation of benefits/remittance; an ERA is the electronic file used for automated posting and reporting.
What does reconciliation mean in billing?
Reconciliation means confirming that posted payments and adjustments match remittances and bank deposits, and then resolving any variances.
How do you identify underpayments?
Compare expected allowed amounts to paid amounts, review adjustment reasons, and track payer trends to decide when follow-up or appeals are worthwhile.
Why do deposits not match the remittance total?
Differences can happen due to offsets/recoupments, multiple ERAs per deposit, missing remittances, or posting errors. Reassociation and variance logs help resolve this.
What are CARCs and RARCs?
They are standardized codes used on remittances to explain claim adjustments and remarks. They help route denials, reductions, and patient responsibility correctly.
How often should a practice reconcile payments?
Many practices reconcile deposits to postings daily or weekly, then do a fuller month-end reconciliation for reporting and A/R aging accuracy.
Can payment posting be automated?
Yes - many systems support automated ERA posting, but you still need controls for exceptions, denials, offsets, and underpayment review.
What should be included in a monthly close report?
Total payments, total adjustments by reason, refunds, unapplied cash, A/R aging by payer, and a list of unresolved variances.
What do you need from our clinic to start?
Payer portal/clearinghouse access (where applicable), adjustment/write-off rules, refund approval workflow, and reporting expectations.
Does payment processing include patient payments too?
It can. A complete reconciliation process includes patient payments, refunds, and unapplied balances so the ledger matches actual cash activity.
Ready to Keep Your Payments Accurate and Balanced?
Let’s walk through your current workflow and show you how we can support your practice.
Your billing should be as reliable as your care.
