Medical Billing Claim Payment Turnover: Complete 2026 Guide
Medical billing for providers isn’t just about submitting claims, it’s about how quickly and consistently money comes back into your practice. Claim payment turnover determines whether you’re paying staff comfortably or constantly chasing balances.
This guide breaks down how long medical claims really take to get paid, what slows them down, and how California practices can shorten that cycle without burning out their staff.
How long does it take to get paid on a medical claim?
To get paid on medical claims, for most California healthcare providers, claims take 30–90 days to get paid from the date of service. Clean electronic claims can pay in as little as 14–30 days, while denied or improperly submitted claims often stretch past 90 days and many are never fully recovered. Faster claim payment turnover depends on accurate credentialing, clean claim submission, payer follow-up, and timely denial management.
Table of Contents
What Is Claim Payment Turnover?
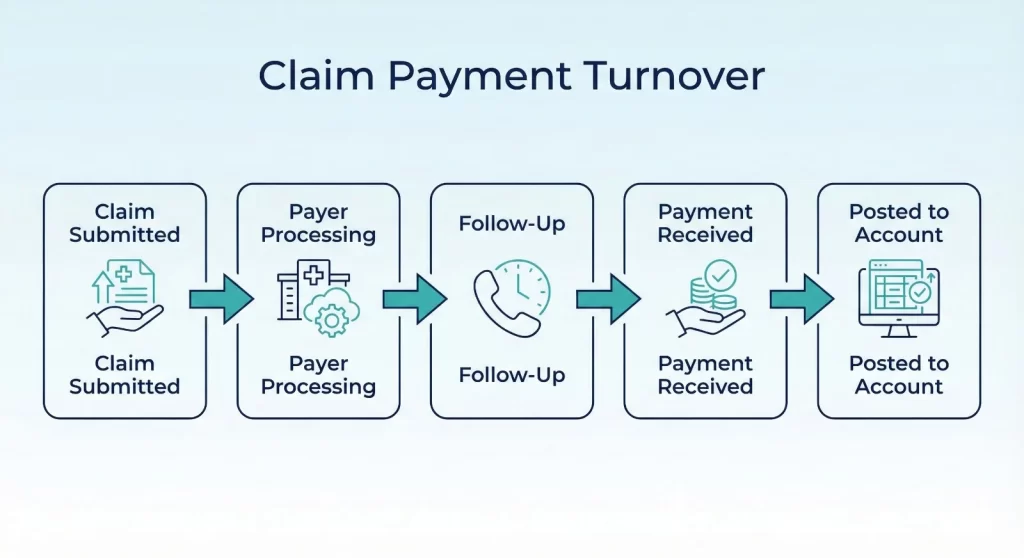 Claim payment turnover refers to the time between providing care and receiving payment from insurance companies. It includes:
Claim payment turnover refers to the time between providing care and receiving payment from insurance companies. It includes:
- Claim creation and submission
- Payer processing and review
- Denials or requests for additional information
- Payment posting and reconciliation
- Payroll becomes stressful
- Rent and overhead eat into savings
- Owners delay hiring or expansion
- Providers start working more for less
Why Claim Payment Turnover Matters for Your Practice
Most small to mid-sized practices operate on thin margins. When payments lag, the financial pressure is immediate. Credentialed vs Poorly Managed Billing| Efficient Billing Process | Delayed Billing Process |
| Payments in 30-45 Days | Payments in 75-120 days |
| Predictable cash flow | Constant Financial uncertainty |
| Low Denial Rates | High rework and write-offs |
| Time spent on patients | Time spent on chasing payers |
| Claim Type | Average Payment Time |
| Clean Electronic Commercial Claim | 14-30 days |
| Medicare Clean Claim | 14-28 days |
| Medi-Cal Claims | 30-60 days |
| Claim with errors or missing data | 60-120+ days |
| Denied Claims requiring appeal | 90-180 days |
What Slows Claim Payments Down
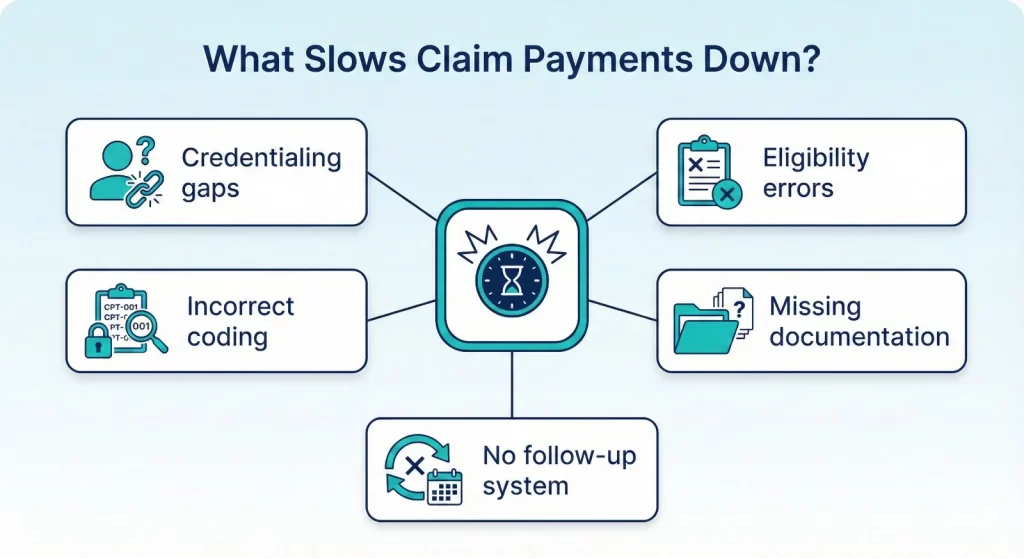 From what we see every day at Claim N Billing, delays usually come from a few repeat issues:
From what we see every day at Claim N Billing, delays usually come from a few repeat issues:
1. Credentialing Gaps
Providers seeing patients before credentialing is finalized often face:- Retroactive denials
- Out-of-network penalties
- Claims that can’t be reprocessed
2. Incomplete or Inaccurate Claims
Even small errors cause big delays:- Wrong NPI or taxonomy code
- Incorrect place of service
- Missing modifiers
- Mismatched provider and location enrollment
3. Poor Eligibility Verification
If benefits aren’t verified correctly:- Claims deny for non-coverage
- Copays aren’t collected
- Appeals drag on for months
4. No Follow-Up System
Many practices submit claims and hope they get paid. Insurance companies don’t work on hope. Without structured follow-up:- Claims fall through the cracks
- Timely filing deadlines pass
- Revenue is permanently lost
Real Revenue Impact: What Faster Turnover Looks Like
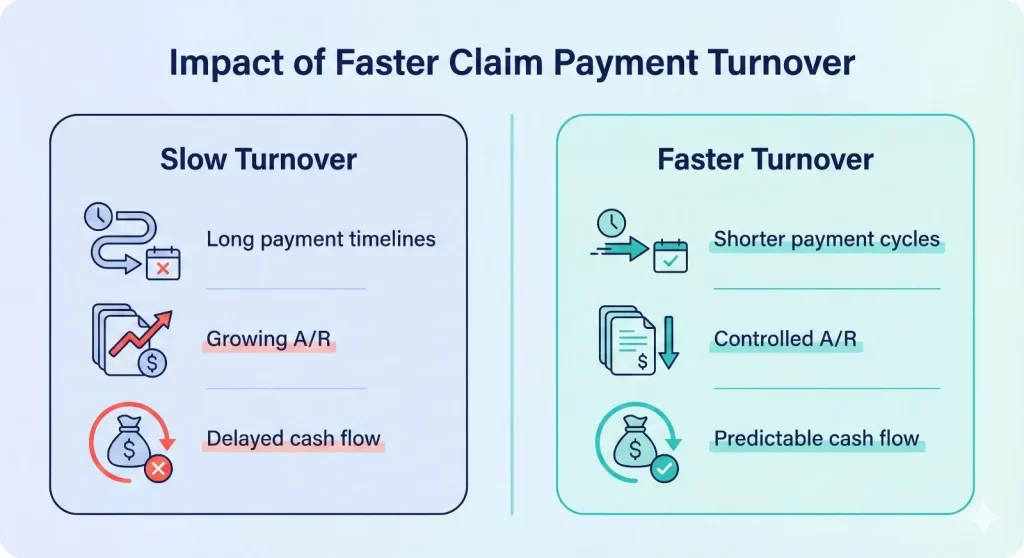
Example: Small California Practice (3 providers)
Before optimization:- Monthly charges: $120,000
- Average days in A/R: 78
- Monthly collections: ~$72,000
- Average days in A/R: 38
- Monthly collections: ~$96,000
Requirements for Faster Claim Payment Turnover
To consistently get paid on time, practices need:Operational Requirements
- Proper insurance credentialing (per provider & location)
- Active CAQH profiles
- Correct payer enrollment setup
- Electronic claims & ERAs enabled
Billing Requirements
- Clean claim rate above 95%
- Daily or weekly claim submission
- Structured denial workflows
- Timely appeals (within payer deadlines)
Management Requirements
- A/R tracking by payer and aging bucket
- Weekly follow-ups on unpaid claims
- Clear ownership of billing tasks
Common Challenges (And Honest Solutions)
“We’re billing in-house, but payments are slow”
In-house billing often lacks:- Time for follow-ups
- Up-to-date payer rules
- Capacity for appeals
“We don’t know what we’re owed”
If you can’t see your aging A/R clearly, neither can your biller. Solution: Transparent reporting that shows exactly where money is stuck.FAQs: Claim Payment Turnover & Medical Billing for Providers
How long should claims take to pay?
Ideally, 30–45 days. Anything consistently beyond that signals process issues.
Is delayed payment normal?
Occasional delays happen. Chronic delays mean lost revenue.
Can old claims still be recovered?
Sometimes, but timely filing limits apply. Many unpaid claims expire permanently.
Does credentialing affect claim speed?
Absolutely. Improper credentialing causes denials, reprocessing delays, and write-offs.
How often should A/R be reviewed?
At least weekly, not monthly.
How Claim N Billing Helps Improve Claim Turnover
At Claim N Billing, we don’t just submit claims, we manage the entire payment cycle.
We work closely with California practices that are tired of guessing when they’ll get paid.
Our Services Include:
- Insurance credentialing & enrollment
- Clean claim submission
- Active denial management
- A/R follow-up and appeals
- Clear, honest reporting
- Ongoing billing optimization
We focus on shortening the time between care and payment, so your practice runs with confidence and not stress.
If credentialing is wrong, billing suffers. That’s why our credentialing services are built directly into our billing workflow.
Contact Claim N Billing
If slow payments are affecting your practice, let’s talk through it, no pressure.
